Why Continence Assessments are Vital for Nursing Home Care
A recent survey published as “Failing the Frail” discovered that only a third of care home staff have attended… Originally posted 2018-08-20 15:05:20.
Continue readingWhat is Biofeedback for Incontinence?
Having weak pelvic floor muscles is a common cause of incontinence. Dysfunction of the pelvic floor… Originally posted 2018-08-08 13:52:31.
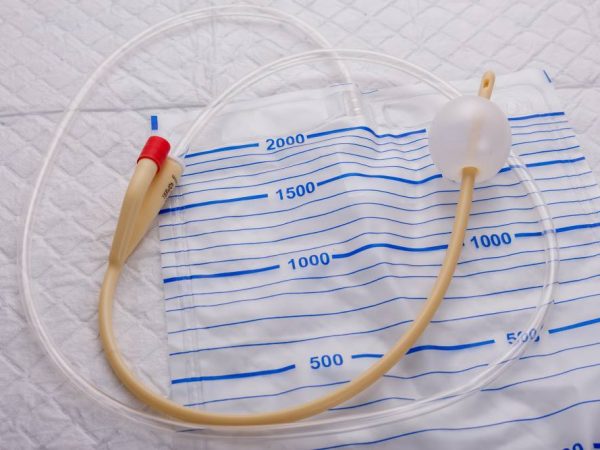
Continue readingLiving with a Urinary Catheter: Tips and Advice
Urinary catheters can be a life-changing solution for many people. Individuals often describe using the products… Originally posted 2018-07-17 15:38:47.
Continue readingCryotherapy for Prostate Cancer: What is It?
Prostate cancer recently overtook breast cancer to become the UK’s third biggest cancer killer. According to Prostate Cancer UK,… Originally posted 2018-05-04 15:47:27.
Continue readingHow to Stop Incontinence Naturally: The Myths and Facts
In extreme cases, surgery methods are necessary in treating incontinence. It can be easy to jump straight to long-term… Originally posted 2018-03-27 15:37:46.
Continue readingBladder Surgery for Stress Incontinence: What are your Options?
The term “bladder surgery” is one which many people edge away from. It can be invasive and extreme. However,… Originally posted 2018-03-23 09:43:43.
Continue reading