What Causes Anal Sphincter Muscle Damage?
Childbirth is the most common cause of damage in women. The incidence of anal incontinence following recognized obstetric anal sphincter injury is estimated at over 60%. 63-year-old Nancy experienced a fourth-degree perineal tear, expanding from the vagina to the rectum. The injury included damage to the anal sphincters. She remembers the tough first days of parenthood, explaining, “I was trying to be a mother while going back in the hospital for surgery. It was overwhelming”. Other women develop symptoms around menopause when the pelvic floor muscles tend to weaken. A common cause of sphincter damage for both men and women is any type of injury to the anus. This injury may be due to accidental damage during an anal or rectal operation, such as haemorrhoidectomy or following an operation for anal fissure or fistula. Damage to the pudendal nerves is another common cause of sphincter muscle damage. The pudendal nerves stimulate the sphincter muscles. Individuals who have experienced damage to the pudendal nerves may find it difficult to know when they are leaking or when they need to defecate. Damage to these nerves can also cause confusion in distinguishing between gas and stool.
Can you Re-Gain Continence after your Anal Sphincter Muscles are Damaged?
If you are suffering from faecal incontinence as a result of anal sphincter muscle damage, do not lose hope that you can regain continence. Your muscles may be weakened; however, this can often be treated through numerous exercises and behavioural techniques. Even in individuals who have structural damage, it is possible for them to regain continence through behavioural treatment. Dr Michael Kamm explains, “there is often an element of reversibility and evidence that a complex combination of factors contributes to continence”. Certain exercises help to strengthen the sphincter muscles. An easy way to locate your sphincter muscles is to pretend you are trying to prevent a bowel movement. When doing this, you should feel the muscles around your anus start to tighten. You should squeeze the muscles for as long as you can, whilst relaxing in between each squeeze. Try to hold for up to 10 seconds and practice this up to 10 times. You can choose between a variety of positions when doing these exercises, for example, sitting, standing and lying down.

Evidence suggests that biofeedback is a successful, minimally invasive method of treating faecal incontinence. This method is painless and safe. In 1974, Engel, Nikoomanesh and Schuster first found biofeedback to be successful in treating faecal incontinence. In this method, patients improve voluntary contraction of the external anal sphincter and puborectalis muscles. The method also aims to improve coordination of the internal and external anal sphincters in response to rectal distention. Biofeedback can be practised with a EMG machine, an anal plug or a recording sponge. Individuals are shown a tracing of the strength and duration of sphincter contraction. Other techniques of biofeedback include manometric techniques or sensory training, which involves placement of an intra-anal balloon. A study in 1997 aimed to evaluate the effectiveness of biofeedback. A case series of patients with faecal incontinence were provided with biofeedback, and 92% of the patients experienced significant improvement with biofeedback. Additionally, advice on resisting urgency alongside the use of medications has been proven to be an effective method.
If you do not see any results from conservative treatment, you should ask your Doctor for surgery recommendations. If your incontinence is severe, an artificial sphincter may be implanted. This method involves placing an inflatable sphincter around the anus. A pump placed inside the body is used to deflate the device, allowing faecal matter to pass through at the appropriate time. For major disruption of the sphincter due to obstetric causes, overlap repair of the sphincter is effective.
Surgery Methods
Sphincteroplasty
This is the most popular bowel incontinence surgery, which reconnects the separated ends of a sphincter muscle. This method is performed at a hospital by a colorectal, gynecological, or general surgeon.
Nonabsorbable bulking agents
Bulking agents can be injected into the wall of the anus to bulk up the tissue around the anus. The bulkier tissues make the opening of the anus narrower so the sphincters can close better. Anesthesia is not needed for this, and the procedure is performed in the office of a health care provider.
Artificial anal sphincter
This is a method that is much less common, and can be performed by a specially trained colorectal surgeon. During this surgery, an inflatable cuff is placed around the anus, implanting a small pump beneath the skin. The person then activates this to inflate or deflate the cuff.

Recommended All in Ones
iD Expert Slip
- Fixation tapes
- Secure and close fit
Range from £4.50 to £16.84
Shop on Incontinence Supermarket
Lille SupremFit
- Hypoallergenic
- Body contoured incontinence pads
Range from £6.55 to £12.63
Shop on Incontinence Supermarket
Lille SupremFit
- Hypoallergenic
- Body contoured incontinence pads
Range from £9.99 to £11.99
Shop on Allanda
Studies suggest that in the UK, constipation and bowel incontinence affects between 3% and 15% of the population. Anal sphincter muscle damage is the most common cause of faecal incontinence.
Why Do We Need Anal Sphincter Muscles?
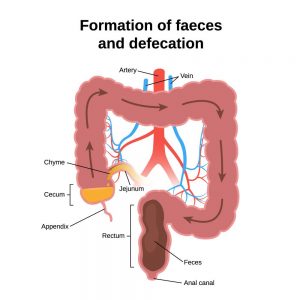
The anal canal is the final segment of the gastrointestinal tract. It has a vital role in defecation and maintaining faecal incontinence. The anal canal begins as a continuation of the rectum and passes in an infero-posterior direction to terminate at the anus. It is divided into three areas: the upper part with the longitudinal folds and the lower portion of the anal opening itself. The sphincter muscles are located in the lower portion and wrap around the anus. The anal canal has a mucous membrane lining, which sends signals to help the brain recognize how full the bowel is. The sphincter muscles in the anal canal are designed to prevent unwanted faeces from coming out of the rectum. Waste products in our body travel to the anal canal from the rectum. The internal sphincter has the job of making sure that the rectum does not open when you are unconscious or sleeping. Nerve responses from the rectum cause the internal sphincter to relax to open the rectal neck. The external muscle contracts, also relaxing a short time after this. This allows defecation.
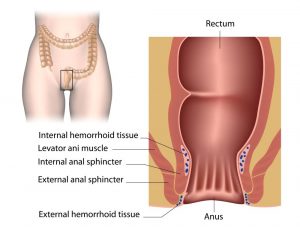
Anatomy of the Anal Canal
Although the sphincters both have the purpose of controlling faecal defecation, they do differ slightly in their design. The internal sphincter is part of the inner surface of the canal and is composed of concentric layers of muscle. It is about 5mm thick, and its lower border is about 5mm from the orifice of the anus. It is a thin, white muscle that wraps around the anal canal and is ring-like in shape. The sphincter muscle is involuntary. We do, however, have some control over the external sphincter. This control is what makes it possible to voluntarily empty your bowels or hold back your stool when you want to. The external sphincter is the muscle that you squeeze when you feel the urge to go to the bathroom but are not near a bathroom yet. This muscle encircles the outside wall of the anal canal and anal opening. If there is no desire to defecate, the external anal sphincter cleverly contracts, mechanically preventing relaxation of the internal sphincter. It also helps the internal sphincter muscle to perform its function. This muscle is a triple-loop system consisting of a top, intermediate and base loop. The external sphincter is the muscle that you squeeze when you feel the urge to go to the bathroom but are not near a bathroom yet.
When these muscles are damaged, however, this method is affected. The muscles may not be strong enough to keep the anus closed and prevent stool from leaking. This, in effect, causes long-term faecal incontinence.
Recommended All in Ones
TENA Flex
- Belted for security
- Available in 3 absorbencies
Range from £13.49 to £27.79
Shop from Incontinence Supermarket
Abena Abri-Form
- Textile Back Sheet
- Discreet and Comfortable
Range from £10.33 to £17.98
Shop from Incontinence Supermarket
Abena Abri-Form
- Textile Back Sheet
- Discreet and Comfortable
Range from £11.99 to £24.57
Shop from Allanda
Originally posted 2018-04-23 15:08:58.

















Stretched sphincter due to bowel surgery. If I try to prevent leakage the faeces just masses and then I can’t pass it .